Stomatitis – causes, treatment, photo
Stomatitis is an inflammatory disease of the oral mucosa. It can manifest itself with various symptoms such as ulcers, redness and swelling. It is a common condition that can occur in people of different ages and have different causes.

Stomatitis is classified according to the International Classification of Diseases (ICD-10 and ICD-11) into several types depending on their causes and characteristics. For example, aphthous stomatitis caused by the herpetic virus and candidal stomatitis caused by fungal infection are common forms of stomatitis classified in the ICD.
| Type of stomatitis | Description |
|---|---|
| Aphthous | The most common form of stomatitis, characterized by the appearance of painful ulcers on the oral mucosa. Usually caused by the herpes virus. |
| Herpetic | It is caused by the herpes virus and is manifested by the appearance of vesicles on the oral mucosa, which then rupture and form ulcers. |
| Candidiasis | It is caused by the fungal infection Candida and is manifested by white plaque on the oral mucosa, as well as ulcers and pain when swallowing. |
| Allergic | Associated with allergic reactions to various substances such as food, medications or toothpaste formulations. May be accompanied by redness and swelling. |
Is stomatitis contagious? Myths and reality
The question of the contagiousness of stomatitis causes many different opinions and myths. Let’s find out how contagious it really is.
Photo of stomatitis:
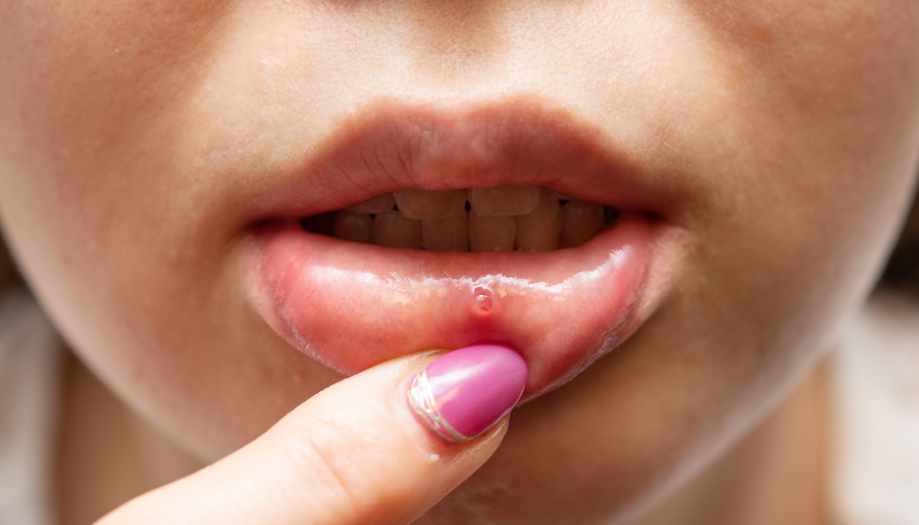
From a medical perspective, most types of stomatitis are not directly contagious from person to person. For example, aphthous stomatitis, the most common type, is not usually transmitted through touch or shared objects. However, some forms of stomatitis, such as herpetic stomatitis, caused by the herpes virus, can be contagious through direct contact with vesicles or sores on the mucous membranes of the mouth.
It is important to remember that the contagiousness of stomatitis depends on its type and cause. Hygienic measures should be taken to prevent the spread of infection, including regular hand washing and avoiding contact with pathogens if possible.
Thus, although some forms of stomatitis can be contagious, most cases do not pose a threat to others, and infection usually occurs if there is close contact with the infected person.
How is stomatitis transmitted?
Stomatitis in adults and children can be transmitted in different ways depending on its type and cause:
- Airborne: Some forms of stomatitis, such as herpetic stomatitis, can be transmitted through the airborne route by contact with droplets of saliva from an infected person.
- Direct contact: Contact with sores, vesicles or discharge on the oral mucosa of an infected person may also result in transmission of stomatitis.
- Common household items: In rare cases, stomatitis can be transmitted through common household items such as cutlery, towels or toothbrushes if they have been used by an infected person.
- Sexual contact: Some forms of stomatitis, such as herpetic stomatitis, can be transmitted through sexual contact during oral sex.
- Vertical route of transmission: In newborns, stomatitis can be transmitted from the mother during passage through the birth canal, especially if the mother has herpetic stomatitis.
It is important to remember that infected people can be contagious as long as they have active symptoms of stomatitis. Therefore, following precautions such as hand cleaning and avoiding close contact with infected areas of the mouth can help prevent transmission of stomatitis.

Duration of stomatitis and factors affecting it
| Factors affecting the duration of stomatitis | Examples |
|---|---|
| Тип стоматита | |
| Aphthous stomatitis: Usually heals within 1-2 weeks | Simple aphthous stomatitis usually heals in 7-14 days, but may be longer if there are complications. |
| Herpetic stomatitis: 2 weeks to 1 month | Herpetic stomatitis can last up to 4 weeks, especially if left untreated. |
| Candida stomatitis: Varies from a few days to a few weeks | In most cases, candidal stomatitis heals in 1-2 weeks with proper treatment. |
| Allergic stomatitis: Depends on the extent of the allergic reaction, usually a few days to a week | Allergic stomatitis can go away quickly if contact with the allergen is eliminated and symptoms are treated. |
| The body’s immune system | | | | | – The state of the immune system can affect the rate of ulcer healing and the reduction of inflammation. | People with weakened immune systems may experience a longer period of stomatitis healing. | |
| Treatment and Care | | | | | – Effective treatment and proper mouth care can shorten the duration of stomatitis. | Using antiviral, antifungal, or anti-inflammatory medications can help speed healing. | |
| General Health and Lifestyle | | | | | – Physical and emotional well-being can affect the duration of stomatitis. | Good nutrition, adequate rest, and reduced stress can contribute to faster recovery. | |
Taking these factors into account helps to assess and predict the duration of stomatitis and take measures to heal it faster.
Stomatitis in adults photo:
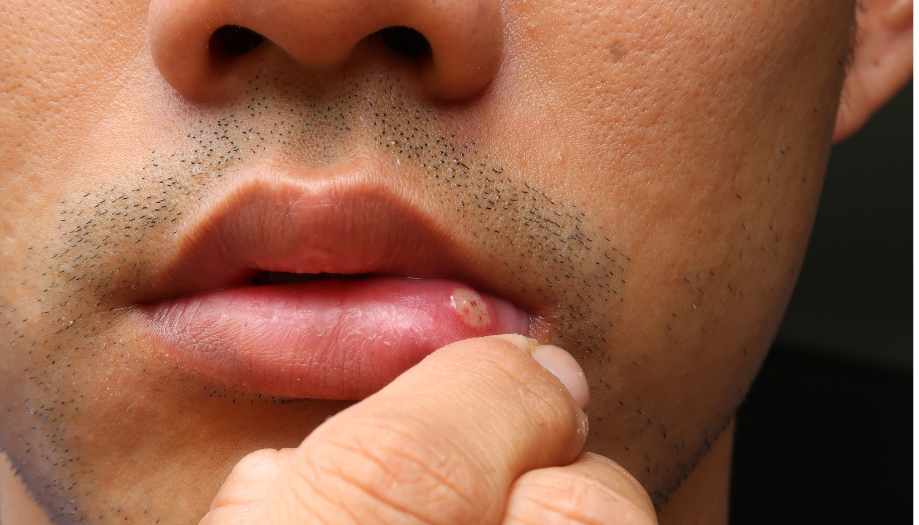
Causes of stomatitis
Stomatitis causes of mouth ulcers:
| Causes of stomatitis | Description |
|---|---|
| Infectious causes | Infectious agents such as viruses, fungi and bacteria play a significant role in causing stomatitis. Here is a detailed overview of infectious causes: |
| Viral infections: | |
| Herpes simplex virus (HSV): One of the most common viruses that causes herpetic stomatitis, manifested as painful sores and vesicles on the oral mucosa. | |
| Herpes simplex virus type 2 (HSV-2): Although this virus is more commonly associated with genital herpes, it can also cause herpetic stomatitis. | |
| Cytomegalovirus (CMV): This virus can cause stomatitis in people with weakened immune systems, especially newborns and people with HIV infection. | |
| Epstein-Barr virus (EBV): Known as the causative agent of infectious mononucleosis, this virus can also cause mouth ulcers. | |
| Fungal infections: | |
| Candida (Candida fungus): This fungus often causes candidal stomatitis, which manifests as white plaque on the oral mucosa, sores, and pain when swallowing. | |
| Bacterial infections: | |
| Streptococci and Staphylococci: Some strains of these bacteria can cause sores and inflammation in the mouth. | |
| Chronic Diseases. | |
| 1. Diabetes mellitus: Patients with diabetes mellitus have an increased risk of developing infections, including stomatitis. High blood sugar levels create a favorable environment for bacteria and fungi to multiply, which promotes oral infections. In addition, reduced body resistance and reduced wound healing in diabetics can increase the risk of stomatitis. | |
| 2. Lupus (systemic lupus erythematosus): This is an autoimmune disease in which the immune system attacks its own tissues, including the oral mucosa. Lupus patients often experience sores and inflammation in the oral cavity, which can lead to the development of stomatitis. | |
| Xerostomia. | Dry mouth, which is common in the elderly, may play an important role in the development of stomatitis. Reduced saliva production in older people can lead to dry mouth, which contributes to irritation of the mucous membranes and increases the risk of stomatitis. Saliva plays an important role in protecting the mucous membranes from bacteria and fungi, so not enough saliva can contribute to the development of infections. Elderly people taking multiple medications may also experience xerostomia as a side effect of the medications, which increases the risk of stomatitis. |
Xerotomy – Photo. Dry mouth in the elderly:
Symptoms of stomatitis
Pain sensations.
Stomatitis pain can be of varying intensity and nature. Patients may experience sharp pain when touching ulcerated formations or when trying to eat. The localization of pain depends on the site of the oral mucosa lesion and may include ulcers on the tongue, lips, cheeks, or gums.
Visual Signs.
Visual signs of stomatitis may include the following changes:
- Edema: Inflammation of the mucous membrane may be accompanied by swelling of the tissues in the area of the lesion.
- Redness: Redness around ulcers indicates an inflammatory process.
- Plaque: White or grayish plaques may form on the surface of ulcers.
- Aphthae (mouth ulcers): They are round or oval ulcers with a red border and a white or grayish bottom.
The size of aphthae can vary from a few millimeters to several centimeters in diameter. The number of aphthae on the oral mucosa can also vary: from one to several dozens.
Precursors to stomatitis may include a burning, tingling or discomfort sensation in the oral mucosa. These precursors may precede the appearance of aphthae by several hours or days.
General symptoms.
In addition to local manifestations, stomatitis can be accompanied by general symptoms:
- Temperature: Some patients may experience a rise in body temperature to 38-39 degrees Celsius.
- Головная боль: Возможны головные боли, особенно при выраженном воспалительном процессе.
- Lymph node enlargement: Lymph nodes in the neck or submandibular fossa may be enlarged and painful when felt.
Types and stages of stomatitis
- Detailed classification by origin:
- Catarrhal stomatitis: caused by irritation of the oral mucosa, most often due to chemical irritants or trauma.
- Traumatic stomatitis: caused by mechanical damage to the mucous membrane, such as a bite or trauma from orthodontic constructions.
- Allergic stomatitis: results from an allergic reaction to certain products or substances, such as foods or medications.
- Classification by duration of course:
- Acute stomatitis: has an abrupt onset and short duration of treatment.
- Chronic stomatitis: characterized by a long course and frequent exacerbations.
- Classification by depth of lesion:
- Superficial stomatitis: affects the upper layers of the mucous membrane and manifests as redness and swelling.
- Aphthous stomatitis: characterized by the formation of aphthae on the mucous membrane, which can be painful and cause discomfort.
- Ulcerative stomatitis: accompanied by the formation of deep ulcerative defects on the mucosa.
- Localization of stomatitis:
- Language
- Gums
- The sky
- Throat
- Lips
- Cheeks
- Classification by area of distribution:
- Single stomatitis: the lesion is limited to a single focus in the oral cavity.
- Multiple stomatitis: there are several foci of mucosal lesions.
- Classification according to the nature of inflammation:
- Superficial forms: characterized by lesions of the upper layers of the mucous membrane and mild symptoms of inflammation.
- Deep forms: inflammation spreads to the deep tissues of the oral cavity and is accompanied by more pronounced symptoms.
Diagnosis of stomatitis
Stomatitis is diagnosed and treated by dentists or dentists. In some cases, consultation with specialized specialists such as an immunologist or allergist may be required, depending on the nature of the lesion.
The doctor’s examination begins with a history, including questions about symptoms, duration of the disease, medications taken, and medical history. The doctor then performs a visual inspection of the oral cavity, assessing the external signs of stomatitis and its localization.
In most cases, laboratory tests are not required to diagnose stomatitis. However, in some situations, the doctor may order a blood test to assess the general condition of the body or a scraping of the affected area to detect possible infections or fungal infections.
- Clinical blood work ( usually 1 to 3 days ).
- Biochemical blood test ( usually 1 to 3 days ).
- Microscopic examination of scrapings from the affected area ( usually 1 to 5 days ).
Treatment of stomatitis with pharmacy remedies
A variety of pharmacy remedies are commonly used to treat stomatitis, including medications to relieve pain, fight infection, and products aimed at reducing inflammation and speeding ulcer healing. Here’s an overview of the main treatments:
- Anesthetic agents:
- Mouthwashes with antiseptic solutions (e.g., chlorhexidine) to reduce pain and inflammation.
- Use of anesthetic gels and sprays based on anesthesin or benzocaine for local anesthesia.
- Antimicrobials:
- The use of antimicrobials, such as chlorhexidine solutions or chlorhexidine-based preparations, to control bacterial infection.
- Antifungal drugs:
- Use of antifungal ointments or solutions (e.g., nystatin, candistatin) to treat fungal stomatitis.
- Противовирусные препараты:
- Use of antiviral agents (e.g., acyclovir) to treat herpetic stomatitis.
- Antihistamines:
- Use of antihistamines (e.g., diphenhydramine) to reduce itching and allergic reactions in cases of allergic stomatitis.

Table with dosages and approximate prices
| The drug | Dosage | Approximate price (in UAH) |
|---|---|---|
| Chlorhexidine | Dissolve with water in a ratio of 1:1 and rinse the mouth 2-3 times a day | 40-80 |
| Бензокаиновый гель | Apply a thin layer to the affected area 2-3 times a day | 80-150 |
| Nystatin ointment | Apply a thin layer to the affected area 2-3 times a day | 30-70 |
| Acyclovir | Apply the cream to the affected areas 5 times a day | 100-200 |
| Diphenhydramine | Take 1-2 tablets 2-3 times a day | 120-150 |
Prices may vary by region and pharmacy network. It is recommended that you consult your doctor or pharmacist before using any medicine.
Hormone therapy when other methods are ineffective
When other treatments fail, hormone therapy may be considered. Hormonal medications may be prescribed as topical applications (e.g., hormonal ointments or sprays) that help reduce inflammation and accelerate ulcer healing.
Physiotherapy (laser therapy)
Laser therapy is widely used in the treatment of stomatitis. Laser exposure helps to reduce inflammation, stimulates healing of ulcers and reduces pain. This method is safe and effective and can be recommended as an additional procedure to the main treatment.
| Laser type | Technology | Wavelengths (nm) |
|---|---|---|
| Diode lasers | Diode | 810 – 980 |
| Erbium yttrium aluminum garnium (Er) and erbium chromium (Er,Cr) | Crystalline | 2780 – 2940 |
| Carbon dioxide gas (CO2) | Carbon dioxide | 9300 – 10600 |
| Intense Pulsed Light Lasers (IPL) | wide range | 500 – 1200 |
| LED therapy | LED | 400 – 700 |
Immune strengthening as an important part of treatment
Strengthening the immune system plays a key role in the fight against stomatitis. Regular intake of vitamins and minerals, as well as a healthy lifestyle with a balanced diet, adequate rest and physical activity are ways to improve the immune system. It is also important to avoid stressful situations, as stress can negatively affect the immune system.
Nutrition and lifestyle recommendations
In stomatitis, it is recommended to follow a soft diet, excluding spicy, acidic and hard foods that can irritate the oral mucosa. Meals should be eaten in small portions, avoiding hot and very cold dishes. It is also recommended to stop smoking and avoid contact with irritating substances such as alcoholic beverages.
Treatment of somatitis by folk methods
Folk ways to treat stomatitis are often used in addition to mainstream medical treatment. Here are some common folk methods:
- Mouthwash with herbal decoctions:
- Rinsing your mouth with decoctions of herbs such as chamomile, sage, calendula or plantain can help reduce inflammation and speed healing of sores.
- Use of honey:
- Honey has anti-inflammatory and antimicrobial properties. Applying honey to the affected areas of the oral mucosa can help in reducing pain and inflammation.
- Treatment with honey and banana peel:
- Mixing honey with the pulp of a banana and applying this mixture to ulcers can help heal them.
- Application of aloe vera:
- Aloe vera juice has anti-inflammatory and healing properties. Rinsing your mouth with aloe vera or applying it to sores can help speed up the healing process.
- Use of soda:
- Rinsing your mouth with a baking soda solution (1 teaspoon of baking soda per glass of warm water) can help relieve inflammation and pain.
- Tea tree oil uses:
- Tea tree oil has antiseptic properties. Applying a small amount of oil to affected areas can help fight infection and speed healing.
It is important to consult a doctor before using folk remedies, especially if you have any medical conditions or allergies.
Stomatitis in children

Pediatric stomatitis has its own characteristics that differ from the manifestations in adults. Here are some of them:
- Frequency of occurrence: Children are more susceptible to stomatitis due to a less developed immune system and lack of hygiene at a younger age.
- Types of stomatitis: Herpetic, candida and aphthous stomatitis are common in children.
- Symptoms: Children may experience pain and discomfort when eating and talking, as well as loss of appetite, irritability and fever.
How to recognize stomatitis in a child?
You can identify stomatitis in a child by the following signs:
- Ulcers and sores: The presence of painful ulcers and sores on the mucous membrane of the child’s mouth.
- Redness and swelling: Inflammation and swelling of the mucous membrane, sometimes with white plaque.
- Pain and discomfort: The child may complain of pain and discomfort when eating, speaking, or even just touching the sores.
How do the treatments differ between children and adults?
Treatment methods for stomatitis in children and adults may differ in the following aspects:
- Medication dosage: Children require more careful dosing of medications, taking into account their age and weight.
- Medication form: For children, special forms of medication, such as syrups or baby powders, may be used to make it easier to take.
- Use of alternative methods: Given the more delicate mucous membranes in children, alternative treatments such as folk remedies may be preferable.
Treatment of stomatitis in children requires special attention and a gentle approach, so it is recommended to consult a doctor for advice and prescribe the right treatment.
Prevention of stomatitis
Prevention of stomatitis plays a key role in maintaining oral health. Here are some recommendations for preventing this unpleasant disease:
- Maintaining oral hygiene: Regular brushing and flossing twice a day can help reduce the risk of stomatitis by removing bacteria and food debris.
- Avoiding traumatic situations: Try to avoid traumatizing the oral mucosa, such as biting down on a sharp or large piece of food.
- Good nutrition: A balanced diet rich in vitamins and minerals helps to strengthen the immune system and maintain mucosal health.
- Avoiding irritating foods: Limit your intake of foods that can irritate the mucous membrane, such as spicy, acidic or fried foods.
- Stress control: Stress can weaken the immune system, increasing the risk of developing stomatitis. Practice relaxation techniques such as yoga or meditation to reduce stress.
- Dental visits: Regular visits to the dentist can help detect problems early and prevent the development of stomatitis and other oral diseases.
- Avoiding contact with infected people: Stomatitis can be transmitted through contact with infected mucous membranes or through shared objects such as cutlery. Therefore, try to avoid close contact with sick people and do not use their personal hygiene items.
If these guidelines are followed, you can significantly reduce the risk of stomatitis and keep your oral health at a high level.

Frequently Asked Questions about Stomatitis (FAQ)
What is stomatitis, causes of occurrence?1. What is stomatitis, causes of occurrence?
- Stomatitis is an inflammatory disease of the oral mucosa caused by various factors, including infections, trauma and others.
Stomatitis in adults: symptoms and signs?2. Stomatitis in adults: symptoms and signs?
- Symptoms of stomatitis in adults include pain, sores and aphthae, redness and swelling of the oral mucosa, and possible increase in body temperature.
Photo of stomatitis and what are its varieties?3. Photo of stomatitis and what are its varieties?
- Stomatitis photos can show different forms and types of the disease, including herpetic stomatitis, aphthous stomatitis, and other types accompanied by characteristic mucosal changes.
Stomatitis in adults: treatment at home what?4. Stomatitis in adults: treatment at home what?
- Home treatment for adult stomatitis may include rinsing the mouth with saline or baking soda solutions, using antiseptic solutions, and applying topical analgesics to relieve pain.
How to cure stomatitis quickly and prevent its recurrence?5. How to cure stomatitis quickly and prevent its recurrence?
- To bquickly cure mouth ulcers, it is recommended to follow the rules of oral hygiene, avoid traumatic factors, eat right and use the treatment recommended by the doctor.
What are the possible complications of stomatitis?6. What are the possible complications of stomatitis?
- Possible complications of stomatitis include infections, pain, eating disorders, increased stress, recurrences, and side effects from treatment.
When should I see a doctor for stomatitis?7. When should I see a doctor for stomatitis?
- If stomatitis does not go away within a few days, is accompanied by severe pain or other unusual symptoms, you should see a doctor for professional advice and treatment.
What precautions should be taken to prevent stomatitis?8. What precautions should be taken to prevent stomatitis?
- To prevent stomatitis, it is recommended to practice good oral hygiene, avoid traumatic factors, maintain a healthy lifestyle including a balanced diet, and visit the dentist regularly for preventive checkups.
What are the causes of stomatitis in adults and how can they be prevented?9. What are the causes of stomatitis in adults and how can they be prevented?
- The causes of adult stomatitis can be varied, including infectious, traumatic, allergic, and other factors. To prevent them, it is important to avoid contact with infected people, avoid traumatic situations, and maintain a healthy immune system.
What are the folk remedies for stomatitis?10. What are the folk remedies for stomatitis?
- Some folk remedies such as chamomile, eucalyptus oil, honey and propolis can help in alleviating the symptoms of stomatitis due to their antiseptic and anti-inflammatory properties.
How is stomatitis in children treated?11. How is stomatitis in children treated?
- Treatment of stomatitis in children involves mild antiseptic mouthwash solutions, topical analgesics and anti-inflammatory medications that are safe for use in children.
What are the complications of stomatitis in children?
- У детей стоматит может вызвать те же осложнения, что и у взрослых, включая инфекции, болевые ощущения, расстройства питания и повышенный стресс. Поэтому важно обратиться к врачу при появлении любых необычных симптомов.
Можно ли самостоятельно лечить стоматит у детей и взрослых?
- Да, в большинстве случаев стоматит можно успешно лечить в домашних условиях, используя мягкие антисептические средства, анальгетики и другие методы симптоматического лечения. Однако в случае сильных болей или неэффективности самолечения следует обратиться к врачу.
Где можно найти фото стоматита у взрослых?
- Фото стоматита помогут вам определить это заболевание. Найти изображения, чтобы узнать, как выглядит стоматит у взрослых возможно на профильных сайтах клиник и на форумах.
В данной статье Coolaser Clinic раскрыла основные аспекты стоматита, включая его причины, симптомы, методы диагностики и лечения. Стоматит может проявляться различными способами и иметь разнообразные причины, от инфекционных агентов до хронических заболеваний и травматических факторов. Важно помнить, что своевременное обращение к профильному врачу и правильно подобранное лечение способствуют быстрому выздоровлению и предотвращению осложнений.
Если у вас возникли первые признаки стоматита, такие как язвочки, покраснение или болезненность в области рта, рекомендуется немедленно обратиться к стоматологу или терапевту. Только квалифицированный специалист сможет провести точную диагностику и назначить эффективное лечение, подходящее именно в вашем случае.
Источники: